

imPACT: September 2019
Message from the Chair

Welcome to the inaugural issue of imPACT, the official newsletter of the Pulmonary Fibrosis Australasian Clinical Trials (PACT) network! Never before has there been such an exciting time in the field of pulmonary fibrosis research. The new antifibrotic treatments are well established on the therapeutic map and there is real momentum driving the development of new, potentially even more effective, breakthrough treatments. The PACT Steering Committee is delighted that Australasia is at the forefront of these advances, with many Australian and New Zealand patients already participating in the latest clinical trials, and our researchers and clinicians driving innovation and discovery.
PACT’s mission is simple – we connect individuals to create a vibrant community of patients, families, loved ones, clinicians and researchers who all share the common goal of defeating pulmonary fibrosis by sharing reliable and up-to-date information about pulmonary fibrosis research. PACT is the result of a powerful collaboration between the Centre for Research Excellence in Pulmonary Fibrosis, funded by the National Health and Medical Research Council, and Lung Foundation Australia. On behalf of the PACT Steering Committee I would like to thank Mark Brooke, LFA’s CEO, for the tremendous support that he and his team have provided to ensure that PACT achieves its mission.
Now that Pulmonary Fibrosis Awareness Month is upon us, the timing could not be more perfect to launch imPACT. Over coming months, we very much look forward to sharing with you the latest in pulmonary fibrosis clinical trials, giving you the low down on what makes some of our lead researchers tick, and introducing you to new PACT/CRE-PF initiatives such as our consumer advisory group. I very much hope you enjoy this first issue of imPACT!
Prof Dan Chambers
PACT Chair
Message from the CRE-PF
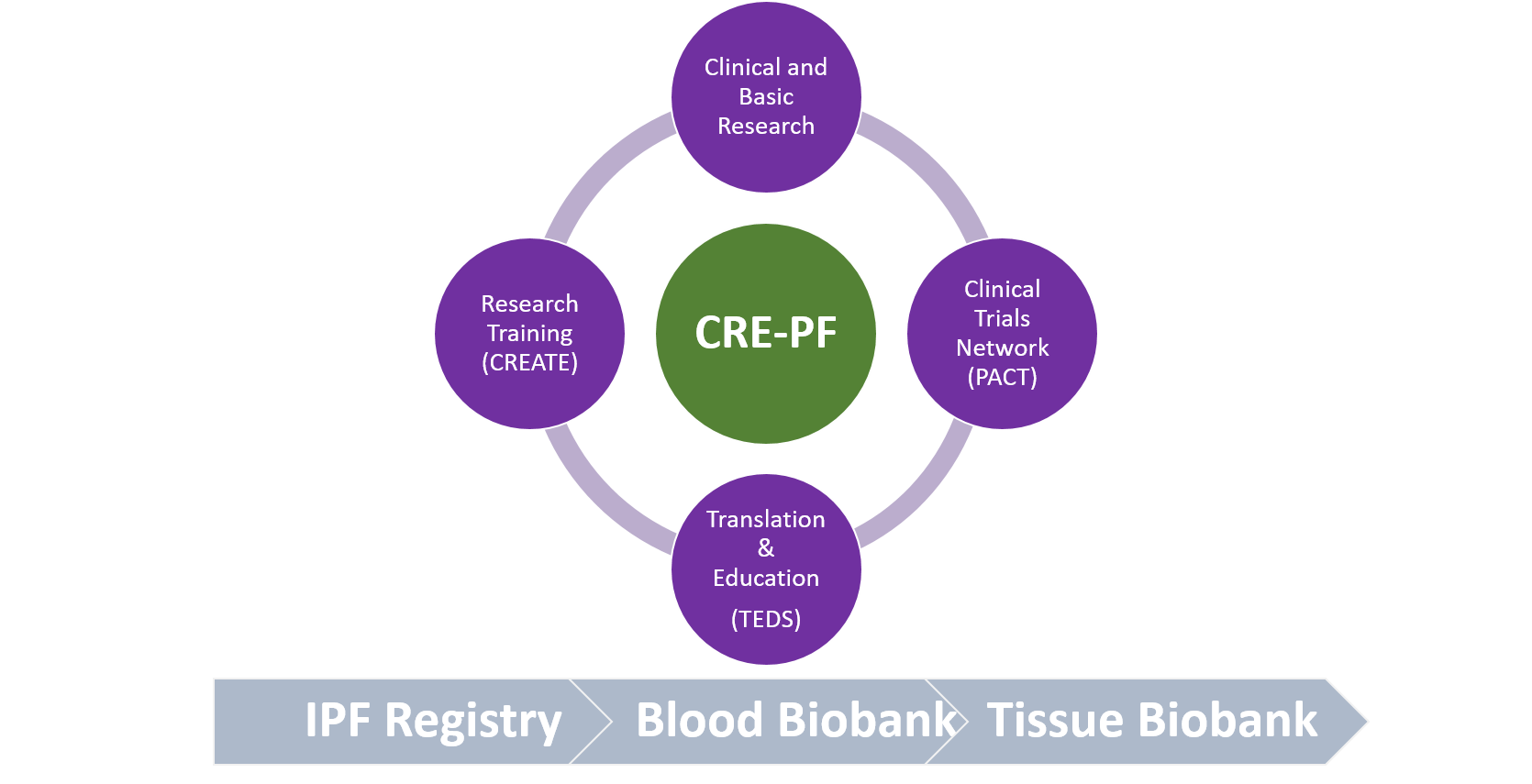
Funded in 2017 by the Australian National Health and Medical Research Council, our Centre of Research Excellence in Pulmonary Fibrosis (CRE-PF) aims to build research capacity in this area. The CRE-PF enables a nationally-coordinated, clinically-focused research program to address the urgent need for more effective, personalised approaches to identify and better manage fibrotic lung diseases, as well as to educate the public and train future generations of researchers in PF.
To do this, the CRE-PF has developed a number of Research Platforms, including PACT, as well as the Australian IPF Registry (AIPFR), a national blood and tissue biobank for PF, a program for Translation, Education and Support (TEDS) and the CRE Advanced Training Environment (CREATE) for research training. The CRE-PF has worked together with Lung Foundation Australia and the Thoracic Society of Australia and New Zealand to develop and maintain these platforms in a sustainable fashion. All our discovery science, clinical and translational research streams are fundamentally based upon these platforms. We are proud to present such a true bench-to-bedside program.
Yours sincerely,
A/Prof Tamera Corte (CIA for CRE-PF)
Grant-in-Aid Winner Announced
The inaugural PACT Grant-in-Aid for Investigator Led Pulmonary Fibrosis Clinical Research, valued at $30,000, was awarded to Dr Lauren Troy from Royal Prince Alfred Hospital in Sydney. Lauren’s award will support her research into better ways of diagnosing PF, building on the world-first COLDICE study of cryobiopsy in PF. Read more about Lauren and her ground-breaking research in ‘Five Minutes with a Pulmonary Fibrosis Researcher’,below. This award will be offered again in 2020.

Dr Lauren Troy, Lead Investigator on the COLDICE Study and recipient of the inaugural PACT Grant-in-Aid for Investigator Led Pulmonary Fibrosis Clinical Research, sat down with the PACT team to talk about the study, including how it started and what the support of the PACT Grant-in-Aid will mean for this research.
Tell us a bit about yourself and why you chose PF as your research area:
I have worked in the Department of Respiratory Medicine at Royal Prince Alfred Hospital since 2009. I was fortunate to be there at the start of the RPAH Interstitial Lung Disease (ILD) Clinic, set up in 2011 by Dr Tamera Corte. Around that time, a lot of exciting changes were occurring globally in the field of pulmonary fibrosis and ILD in general. Once I finished my training, the decision to do further research in this area was very easy. I completed my PhD in pulmonary fibrosis related research at the end of 2016 and have continued working in the clinic ever since. Along the way, I decided to expand my training in respiratory diagnostic and interventional procedures, including learning how to perform cryobiopsies for ILD diagnosis. Over the past 3 years, my interests in ILD and respiratory diagnostics have come together in the COLDICE Study.
Describe your trial in a couple of sentences:
The COLDICE (Cryobiopsy versus Open Lung biopsy in the Diagnosis of Interstitial lung disease allianCE) Study is looking at how the cryobiopsy compares with the traditional surgical lung biopsy for ILD diagnosis. The cryobiopsy is a new technique for taking small samples of lung tissue through the airways, rather than through the chest wall, as is the current approach for surgical biopsies. The samples from cryobiopsy are much smaller than surgical biopsies, so it is not yet known if they are as accurate or reliable. Our study will help to answer this question, and hopefully inform clinicians when diagnosing their patients.
Tell us how this trial/ came about:
The COLDICE Study came about in 2015 when a few of us in the ILD Clinic heard about cryobiopsy being used with enthusiasm in some European hospitals. I remember having a chat over a team coffee about whether cryobiopsy results were accurate. We decided that we would create a study to answer the question. My colleague Dr Edmund Lau and I travelled to Tubingen in Germany to be trained in this new technique. We then collaborated with Dr Jonathan Williamson from Liverpool Hospital in Sydney, for further training. There was a lot of interest from many Australian hospitals. In the end, 9 sites took part in the study, which finished recruiting in April 2019. There was interest from New Zealand and American sites to join as well, but for logistical reasons it ultimately wasn’t possible. The study has been mentioned at international conferences and results are now awaited by the ILD community.
What do you hope this trial will achieve?
We hope to answer the question of whether cryobiopsies are a suitable alternative to surgical lung biopsies for ILD diagnosis. This is an important question, as the surgical lung biopsies carry some risk. Many ILD patients are too unwell to have a surgical biopsy so their diagnosis remains uncertain. This can impact on treatment decisions and outcomes. If there is a safer, reliable way to make a diagnosis, this would be preferable for many patients. Our preliminary results are very encouraging and support the role of cryobiopsy.
What has been the biggest challenge of the trial so far?
Where to start?! The challenges of the study have been more than offset by the tremendous support of many people. Aside from connecting with many clinicians and researchers in the fields of ILD and respiratory diagnostics, this study has shown me the generosity of people suffering with pulmonary fibrosis. I have heard over and over again how people wanted to participate to help others. By participating in the study, they felt strongly that they could benefit other sufferers of these diseases.
The people working on this trial are:
More than 50 people from around Australia and internationally have collaborated with us on this study. Aside from Edmund Lau, Tamera Corte and Jonathan Williamson, other key people have been Chris Grainge from John Hunter Hospital in Newcastle, Wendy Cooper and Annabelle Mahar from RPAH, Jeffrey Myers from Ann Arbour, Michigan, Ganesh Raghu from University of Washington Seattle and Michael Vallely from Macquarie University Hospital. Our study coordinators Tina Lin, Jessica Rhodes and Susanne Webster have been critical for the smooth running of the study and data entry.
What will the support of the PACT Grant-in-Aid mean for your clinical research/trial?
We are really grateful to receive the PACT Grant-in-Aid funding, which we plan to use for further research into specialised diagnostic testing in interstitial lung disease (ILD). We are hoping to extend the findings of the COLDICE study, incorporating new technologies such as digital pathology, micro-CT scanning and molecular sequencing. The field of ILD diagnosis is evolving at a rapid rate and our aim is to contribute to this in some way.

What do you see as the biggest evidence gaps in PF care? What are the clinical research priorities?
Large-scale international research is focusing on stopping the progression of pulmonary fibrosis, or at least slowing it down. Whilst these are very important things to target, there are many unmet needs of people living with these diseases. Quality of life and symptom control are relevant to all ILD sufferers and need to be the focus of current and future research.
Wrap-up of the 4th Biennial Australian Rare Lung Disease Short Course
The 4th Rare Lung Disease course has just drawn to a close. Supported by Lung Foundation Australia, the course was a sellout with delegates gaining access to the most up-to-date advances in the treatment and management of rare lung diseases, including Pulmonary Fibrosis (PF). Delegates heard ground-breaking presentations from national and international experts, including hot-of-the-press information about the much anticipated INBUILD and COLDICE trials, with results for these much anticipated trials to be announced at the upcomingEuropean Respiratory Society (ERS) Conference in Madrid in late September. International experts Kevin Brown (National Jewish Health, Denver), Ivan Rosas (Brigham and Women’s Hospital, Boston and Principal Investigator for the TRAIL study) and Sujal Desai (Royal Brompton, London) entertained and enlightened with their insights into the future of PF care and research. The conference concluded with an inspiring vision for the future of PF research in Australasia from Gary Anderson (Uni Melbourne). As one of our most celebrated drug discoverers, Anderson discussed a more sophisticated and personalised understanding of the causes of PF.

One of the real innovations at this year’s course was the Identifying Research Priorities for Pulmonary Fibrosis Workshop. Consumers and the community offered unique and valuable insights into PF that will help guide the direction that research should be heading. By sharing their opinions as a someone living with PF, a carer, a healthcare professional or researcher, delegates were able to help the CRE-PF identify what research questions matter most.
Interstitial Lung Disease Patient Education Day
Lung Foundation Australia invited patients, their families and friends to join us to hear the latest evidence in self-management and tips for living well with Interstitial Lung Disease (ILD). Lung Foundation Australia were excited to present both international and local experts in the field, including Professor Kevin Brown.


European Respiratory Society International Congress
28 September - 2 October Madrid
This year’s ERS meeting is one of the most hotly anticipated ever for PF research. Results of some of the most important PF trials ever conducted, including INBUILD (Nintednaib for progressive PF), the prifenidone in unclassifiable ILD trial and our own COLDICE study, will all be released at ERS. See you there!
Register
Membership
The PACT network continues to build our membership and welcomes new members across all aspects of pulmonary fibrosis clinical research, care and support. We invite you to encourage your colleagues to join our growing community.
Become a member
Find a trial
PACT has nine active trials listed on our website. These trials are currently recruiting in locations across Australia and New Zealand.
Find a trial